The “fourth trimester” or postpartum period
The postpartum period, sometimes referred to as “the fourth trimester” is the period of time someone experiences after delivering a baby. It can be divided into at least three distinct phases depending on the length of time after delivery.1 When exactly postpartum ends varies depending on the source and doesn’t have a clear definition. One paper suggests the final phase of the postpartum period ends up to 6 months after a baby is delivered.1
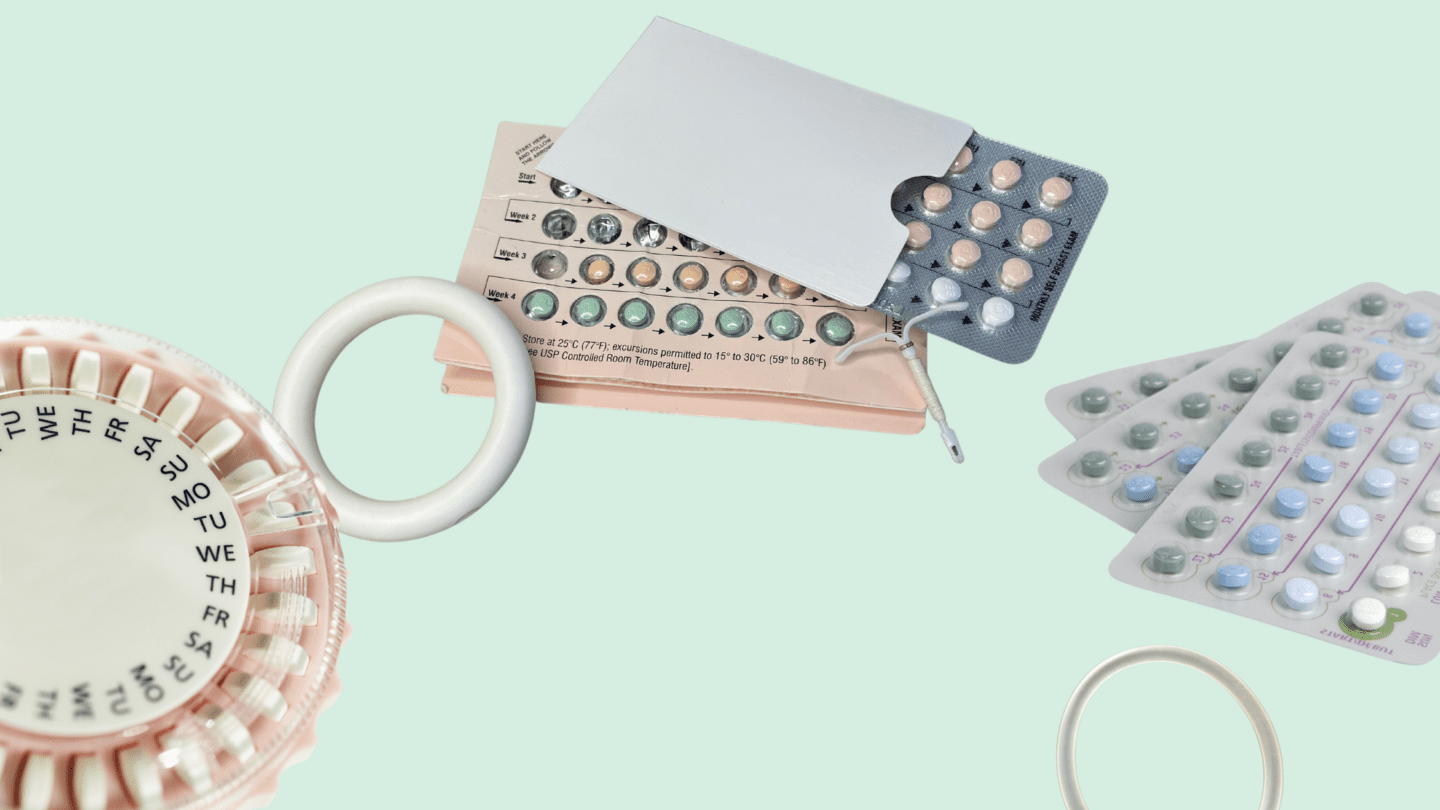
Importantly for your thoughts on , no one can say exactly when you’ll begin ovulating after delivery and you may start ovulating (aka be able to become pregnant again) before you want to conceive. In other words, since it’s possible to ovulate before your first period after having a baby, you may not know when after delivery you become fertile again.2 For this reason, or many others, many postpartum individuals may want to use .
You definitely can be on during your postpartum time, there are just a few special considerations and things to know about during this unique time of your life.
What is happening to your body postpartum?
Let’s first talk about what is going on with your body during the postpartum period. Bottom line: a LOT is going on. Read on for the details.
The first phase of the postpartum time is called the acute or initial phase and includes up to the first 12 hours post delivery. There are lots of changes happening to your body during this time and potentially dangerous complications can occur.1 This is probably not the best time to think about . During this phase, your time is better spent trying to rest, recover and get to know your baby. Most likely, these 12 hours will fly by.
The second phase of postpartum is the subacute, aka the “short term”, and includes up to the first 6 weeks after delivery. During this time there are still many changes happening in your body as it adjusts to supporting a baby outside rather than inside. These changes include:1,3-6
- Uterus returns to its original size
- Breast changes as milk production begins/stabilizes/ends depending on how long breastfeeding is continued
- General physical and mental healing from delivery
- Massive hormonal shifts
- Likely considerable sleep deprivation if caring for a newborn
All of these changes mean that this is the highest risk time for developing postpartum depression, anxiety or general “baby blues”.7 Please seek medical counsel if you think you need it, or just want to talk to someone.
Like what you’re reading? Get the latest straight to your inbox 💌
The final phase of the postpartum period is the longest term phase, sometimes called the delayed phase, and lasts from 6 weeks to 6 months post delivery.1 Some parts of your body will take even longer than six months to return to their pre-pregnant state, and some changes you are probably stuck with forever (for me, it was bigger feet!). Changes during this phase include:1,4,5,8,9
- Breasts and breast milk changes and production stabilizes/continues/ends
- Muscle tone and connective tissues are restoring themselves (aka pelvic floor muscles)
- Post pregnancy hormonal changes continue until your monthly cycle picks back up
Hopefully this time is also seeing better and more sleep, a routine develop and a general feeling of recovering.
Clearly, there is a LOT going on with your biology and life changes after having a baby. So, how does fit into this?
Why use after having a baby?
There are lots of reasons to use after having a baby. Having a baby in your life is a lot of work. Having babies too close together can put the mother and next baby at risk for complications.10 can help with medical issues besides preventing pregnancy. You may want time to reflect and evaluate your family planning plan.
With all of this weighing on your mind, biology has also put you in a tricky situation since you likely will not know when you will become fertile and start ovulating again. Enter, your postpartum options.
Is adyn right for you? Take the quiz.
What are my options after delivery?
First off, if the postpartum woman has puerperal sepsis, no form of is considered safe.11 Puerperal sepsis is when there is an infection of the genital tract within 42 days of childbirth.12 It is among the five most common causes of maternal death worldwide.13 Since it is clearly a very serious condition, we hope that any patient with puerperal sepsis has a support system that can help them focus on recovering and that decisions and actions come later.
Now, if that sentence does not apply to you, then there are few factors that may influence your postpartum choice. Try asking yourself:
- Will I be producing breastmilk when on ? (stay on this page and keep reading!)
- What are my reasons for being on ? (see our post on other medical reasons for )
- How long would I like to be on ? (see our post on the best )
- Is the effectiveness of the method important to me? (see our post on what are very effective options)
The answers to those questions can help you narrow down your options, but there will probably still be options to choose from. Let’s discuss a few specific considerations for this unique time in your life, based on method type.
Combined methods (aka some pills, patch, ring)
The CDC recommends no one start combined hormonal contraceptives during the first 3 weeks after childbirth due to an elevated risk of deep vein thrombosis (DVT).11 DVT is when a blood clot occurs in a deep vein. It is a dangerous condition because the clot can dislodge and relocate to the lungs and interfere with breathing. The risk of DVT is elevated during the postpartum time.
Be particularly aware of this if you already have an elevated risk of DVTs. The CDC says to wait until 6 weeks after delivery if you have enhanced DVT risk factors before starting a combined option.11
To be extra transparent, there is no data that shows combined hormonal contraceptives increase the risk of DVTs in postpartum females. However, the risk of DVTs is known to be elevating during the postpartum time and CHCs can elevate the risk of DVTs in healthy non-pregnant or -postpartum females. The combined risk of these two factors and the seriousness of the condition are enough for the CDC to put out this recommendation.
Overall, six weeks after delivery, your combined hormonal methods are back on the table.
IUDs
An IUD can be a great option postpartum due to their effectiveness and minimal necessary upkeep.
However, you might not want to jump the gun on getting it inserted since an IUD is more likely to fall out if placed right after delivery.2 As mentioned, the rate of expulsion varies with when it was placed.14-15 Even higher numbers were found in a Swedish study, where 44% of hormonal IUDs inserted within 48 hours of delivery were expelled.16
Progestin only methods (other than IUDs)
You might already know that only methods come in a variety of shapes and sizes. These include the mini pill, hormonal IUDs, the arm implant and injections. (Questions about IUDs vs. the implant? Check out more here.)
It is safe to receive either the injection or the arm implant (Nexplanon) right after childbirth. Like IUDs, these long acting methods have minimal upkeep requirements.
Progestin oral contraceptives can also be started right after delivery.2 However, remember that these must be taken at exactly the same time every day to be effective. Read: your sleep-deprived, emotionally exhausted, distracted brain might not be great at remembering this right now.
Multiple studies have found no reliable effect of only contraceptives on lactation.17-18
Overall, the different progestin-only forms have unique advantages or disadvantages, but all are safe for use during the postpartum time.
Other methods
The cervical cap, diaphragm and sponge can be used starting 6 weeks after delivery, according to the ACOG. However, the sponge and cervical cap are much less effective in women who have given birth.2 These are also not considered to be highly-effective methods.
Regarding sterilization– at some hospitals, you can have your tubes tied (tubal ligation) during a C-section. So, if you are considering it, it may be worth asking about before you head to the hospital for delivery, especially if you know you’ll be having a C-section. Otherwise, you have to wait several weeks to do this procedure.
When to start after baby
When you can safely start postpartum depends on the method. Some methods you can start before you leave the hospital.2 But, some providers recommend not putting anything inside your or for the 4-6 weeks after delivery.19 In the US, this often coincides with the recommended postpartum OB/GYN office visit. Your body just did a lot, give it a minute to heal.
If you want to start before the 6 week postpartum time, you can start taking certain pills or have an IUD placed in the hospital before you go home. One caution about IUDs though, there are higher rates of IUD expulsion if the IUD is placed soon after birth. The rate of expulsion varied with the timing of insertion post delivery: 10% when placed within 10 minutes of delivery, nearly 30% when placed between 10 minutes and 4 weeks after delivery and only 1.9% when placed after 4 weeks postpartum.14 Interestingly, these numbers were nearly identical in another study.15
After 6 weeks, most providers say you can be sexually active again. So, this seems like a good time to have a new plan ready to enact if you follow this advice and want to be extra cautious about preventing pregnancy.
How does breastfeeding influence postpartum?
Breastfeeding can elicit many emotions and debates that might be in the back (or front) of your mind if you are reading this article. If you choose to produce breast milk, most options are considered safe, as outlined above. Here are a few extra facts to think about for those who are lactating postpartum.
Lactational amenhorrea method (LAM)
Interestingly, breastfeeding opens up the option for a form of unique to the postpartum period– the lactational amenorrhea method (LAM).
The LAM of can be achieved when you are doing frequent, exclusive breastfeeding (baby is nursing every 4 hours during the day and 6 hours at night). This level of breastfeeding can serve to prevent ovulation, and therefore prevent pregnancy. It is more common in the first six months after delivery.2
The disadvantage of LAM is that you cannot predict when it will stop working and ovulation will begin, so you have no idea when this method will stop being effective.
It is also unclear if pumping your breasts instead of directly having your baby nurse will successfully prevent ovulation and produce an effective LAM.
Warnings
There are a few warnings that we could find specifically regarding and breastfeeding during the postpartum time.
First, combined options should not be taken immediately after delivery. There is a small chance they lower milk supply and so it is suggested that lactating people wait until breastfeeding is well established (often cited as 4-6 weeks) before using these methods of .11
Second, the Australian government suggests that women who are breastfeeding do not use the emergency contraceptive pill containing ulipristal acetate (UPA). They cite the fact that UPA is known to pass to breastmilk and the effect of UPA on an infant has not been studied.20
So, as we’ve seen before, although there are expert recommendations, there’s not much evidence backing them up and more research is needed in this area of reproductive health.
Take a deep breath
This is a unique, wonderful, exhausting, crazy time of your life. There are many options that are safe, effective and simple enough to use during the postpartum time so that you can enjoy it to the fullest.
Ready to find the right for your body? Get started with The Birth Control Test.
-
- Romano M, Cacciatore A, Giordano R, La Rosa B. Postpartum period: three distinct but continuous phases. J Prenat Med. 2010;4(2):22-25.
- ACOG. Postpartum Birth Control. https://www.acog.org/womens-health/faqs/postpartum-birth-control. Accessed 04/2022-06/2022. Last updated and reviewed: November 2021
- Uterus Involution. Cleveland Clinic. https://my.clevelandclinic.org/health/articles/22655-uterus-involution. Accessed 06/2022. Last reviewed 04/01/2022.
- de Holanda AA, Gonçalves AK, de Medeiros RD, de Oliveira AM, Maranhão TM. Ultrasound findings of the physiological changes and most common breast diseases during pregnancy and lactation. Radiol Bras. 2016;49(6):389-396. doi:10.1590/0100-3984.2015.0076.
- Hendrick V, Altshuler LL, Suri R. Hormonal changes in the postpartum and implications for postpartum depression. Psychosomatics. 1998;39(2):93-101. doi:10.1016/S0033-3182(98)71355-6
- Richter D, Krämer MD, Tang NKY, Montgomery-Downs HE, Lemola S. Long-term effects of pregnancy and childbirth on sleep satisfaction and duration of first-time and experienced mothers and fathers. Sleep. 2019;42(4):zsz015. doi:10.1093/sleep/zsz015
- Identifying Maternal Depression. Centers for Disease Control. https://www.cdc.gov/reproductivehealth/vital-signs/identifying-maternal-depression/index.html
- Fukano M, Tsukahara Y, Takei S, Nose-Ogura S, Fujii T, Torii S. Recovery of Abdominal Muscle Thickness and Contractile Function in Women after Childbirth. Int J Environ Res Public Health. 2021;18(4):2130. Published 2021 Feb 22. doi:10.3390/ijerph18042130
- Nygaard IE, Wolpern A, Bardsley T, Egger MJ, Shaw JM. Early postpartum physical activity and pelvic floor support and symptoms 1 year postpartum. Am J Obstet Gynecol. 2021;224(2):193.e1-193.e19. doi:10.1016/j.ajog.2020.08.033
- Conde-Agudelo A, Rosas-Bermúdez A, Kafury-Goeta AC. Effects of birth spacing on maternal health: a systematic review. Am J Obstet Gynecol. 2007;196(4):297-308. doi:10.1016/j.ajog.2006.05.055
- Randel, Amber. CDC Updates Recommendations for Contraceptive Use in the Postpartum Period. Am Fam Physician. 2011;84(12):1422-1425.
- Buddeberg BS, Aveling W. Puerperal sepsis in the 21st century: progress, new challenges and the situation worldwide. Postgrad Med J. 2015;91(1080):572-578. doi:10.1136/postgradmedj-2015-133475
- Maternal mortality. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/maternal-mortality. 19 September 2019. Accessed 06/2022.
- Jatlaoui TC, Whiteman MK, Jeng G, et al. Intrauterine Device Expulsion After Postpartum Placement: A Systematic Review and Meta-analysis. Obstet Gynecol. 2018;132(4):895-905. doi:10.1097/AOG.0000000000002822.
- Averbach SH, Ermias Y, Jeng G, et al. Expulsion of intrauterine devices after postpartum placement by timing of placement, delivery type, and intrauterine device type: a systematic review and meta-analysis. Am J Obstet Gynecol. 2020;223(2):177-188. doi:10.1016/j.ajog.2020.02.045
- Lichtenstein Liljeblad K, Kopp Kallner H, Brynhildsen J. Effectiveness, safety and overall satisfaction of early postpartum placement of hormonal IUD compared with standard procedure: An open-label, randomized, multicenter study. Acta Obstet Gynecol Scand. 2022;101(4):424-430. doi:10.1111/aogs.14331
- Lopez LM, Grey TW, Stuebe AM, Chen M, Truitt ST, Gallo MF. Combined hormonal versus nonhormonal versus progestin-only contraception in lactation. Cochrane Database Syst Rev. 2015;(3):CD003988. Published 2015 Mar 20. doi:10.1002/14651858.CD003988.pub2
- Phillips SJ, Tepper NK, Kapp N, Nanda K, Temmerman M, Curtis KM. Progestogen-only contraceptive use among breastfeeding women: a systematic review. Contraception. 2016;94(3):226-252. doi:10.1016/j.contraception.2015.09.010
- ACOG. A Partner’s Guide to Pregnancy. https://www.acog.org/womens-health/faqs/a-partners-guide-to-pregnancy. Accessed 06/2022. Last updated and reviewed: November 2020.
- Contraception after giving birth. The Department of Health, State Government of Victoria, Australia. https://www.betterhealth.vic.gov.au/health/healthyliving/Contraception-after-childbirth. Last reviewed on 05/17/2018. Accessed 04-06/2022.