Birth control is often thought of only to prevent pregnancies, but it can be used for so much more. Here we recap the basics of your hormones, and explain how can be used to alleviate symptoms of various medical conditions.
What Are Hormones and How Do They Work?
Hormones are chemical messengers that transport signals between organs and tissues in our bodies. They influence many areas of life, from growth and development, to appetite and mood. Hormones are produced in the endocrine glands, which include the pituitary gland, thyroid, adrenal glands, pancreas, , and the testes. Hormones act throughout the body on tissues that have specific receptors for them.1
A number of hormones are reproductive hormones, which organize fertility and sexuality.2 Altering the levels and balance of your reproductive hormones is the basis for methods.
Hormonal Methods
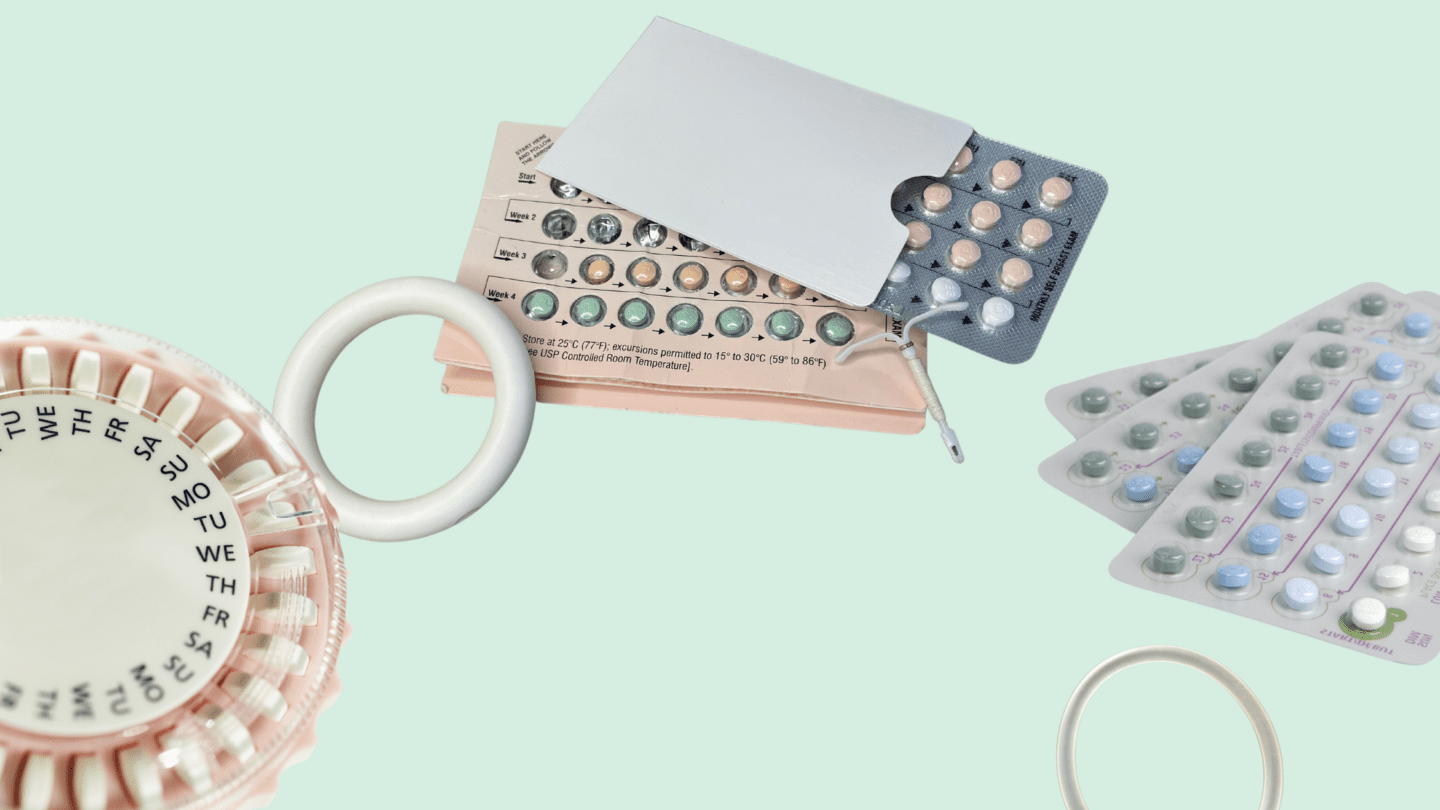
As its name implies, the original intended function of (AKA ) is fairly self-explanatory — it works to prevent pregnancy before it happens. The many methods of can be grouped into different categories, including hormonal and non-hormonal methods. This post focuses on the hormonal methods and how you can use them as medicines for indications other than preventing pregnancy. Here’s a quick recap of options.
Hormonal
Hormonal methods contain an and a or only a . They include:
- Combined pill
- Progestin-only pill (mini pill)
- The patch
- The ring
- The shot
- All other IUDs
- The morning-after pill (emergency contraception)
Just like non-hormonal methods, hormonal birth controls have varying degrees of efficacy.3
Hormonal Contraceptives: More Than Pregnancy Prevention
While can be excellent at preventing pregnancy, it’s not only used to prevent pregnancy. In fact, people have been researching and reporting “noncontraceptive uses” for pills for decades. In some cases, the treats the underlying issue, while other times its mechanism may not be known or it just alleviates symptoms.
58% of people who take the pill use it for a purpose other than pregnancy prevention.4 14% take it exclusively for non-contraceptive purposes.
There are many reasons people take birth control pills, from mitigating the side effects of menstruation like cramping and heavy bleeding, to the treatment of acne and . Please consult with a physician before diagnosing or treating yourself with hormonal birth controls.
Is adyn right for you? Take the quiz.
Hormonal to Improve Medical Conditions
There’s an (unfortunately) common thought that will inevitably cause bad side effects—and that people who take it should just accept this if they want to reap its benefits. This doesn’t have to be the case, and can be tailored for your medical needs and lifestyle.
Due to differences, genetics, and individual preferences, different methods work better for certain people. This is also true when using hormonal contraceptives for “noncontraceptive uses”. Below are just a few examples of situations in which s can be used as therapies for different conditions.
Endometriosis
Endometriosis is a condition that causes the lining of the to grow outside of the . When the lining grows and breaks down, the body can experience swelling and pain, as the tissue is in an area where it was not meant to be. While the exact cause of has not been identified5, genetics and high levels of appear to play a role.
Hormonal birth control pills have been used, with questionable evidence of clinical success⁶ ⁷to treat mostly the pain symptoms of . However, research suggests that progestin-only pills may be more effective8 at treating the pain and bleeding associated with than / combined pills. Additionally, only pills have been shown to reduce the progression of the disease after surgical treatments.7
Although no one type of seems better for patients, multiple options can improve the quality of life for patients with .7,9
Polycystic Ovary Syndrome
Polycystic Ovary Syndrome (PCOS), is a syndrome of hormonal imbalance characterized by irregular periods, signs of excessive s– like acne or facial hair growth– and fluid-filled sacs (immature follicles) in the . To be diagnosed with PCOS, an individual will have evidence of at least two of these three signs of PCOS.
Symptoms of PCOS can be treated with . Combined and progestin-only pills can help to reduce hyperandrogenism symptoms such as facial hair, acne and menstrual dysfunction.7 Therefore, combined hormonal contraceptives are actually considered a first-line medication for PCOS patients.
The best pill to treat the metabolic symptoms often associated with PCOS is unique per patient–different s are better depending on specific metabolic conditions or risks.10 In some PCOS cases, progestin-only pills are safer than the combined pills.10
Migraines
The story with hormonal contraceptives and migraines is somewhat complex. There is evidence that hormonal contraceptive pills that prevent ovulation can prevent migraines caused by decreases in levels.11
For a select group of individuals, caution should be noted when considering pills. Older data showed an increased risk of ischemic stroke in ovulatory patients who regularly had migraines with aura and took birth control pills.11-12 Because strokes can be so devastating, there is a long-standing (and recently upheld12) contraindication for patients who experience migraines with aura and combined pills.
Progestin-only pills have no contraindications related to migraines, and arm implant progestin-only pills may relieve migraine headaches without the hassles of the mini pill.11
Overall, new studies are needed to reflect the major changes in over the past 50+ years.11-12
Like what you’re reading? Get the latest straight to your inbox 💌
Acne
Acne is one of the most commonly treated skin disorders. One meta-study looked at 31 different clinical trials across the world with 12,579 patients in total and found that oral contraceptive pills with multiple different active ingredients helped alleviate acne symptoms. All nine of the placebo-controlled trials evaluated in that study showed improvement in the number of facial lesions, their severity and patient-assessed overall acne compared to the .13
Acne is also a reported potential side effect of hormonal birth controls.
Heavy Menstrual Bleeding
For some people who menstruate, their period comes with constant cramps or pain and excessive bleeding that can lead to fatigue and interference with daily activities.
Heavy Menstrual Bleeding is defined as greater than 80mL of blood lost and is common, affecting potentially 30% of menstruating individuals.7
Hormonal birth controls are not created equal when it comes to treating Heavy Menstrual Bleeding. The best option is levonorgestrel-containing s– they are even FDA-approved for Heavy Menstrual Bleeding. They work well because they thin the endometrial lining so there is less to shed (bleed) during a period. A far second, pills can also be used to decrease blood loss during menstrual bleeding.7
Cancer
Hormonal contraceptive use can reduce the of endometrial and ovarian cancers.
For ovarian cancer, the strongest effect was shown with combined oral contraceptives used for over 10 years, starting before age 35. Interestingly, the effect of use can last up to 25 years after taking the pills!7
For endometrial cancer, levonorgestrel-containing s reduced the risk the most– by 78%14. Combined oral contraceptives also reduced endometrial cancer , again mostly significantly when used for >10 years and when the patient has other risk factors for disease.7
The Right For Your Needs
These are a few examples of how can be optimized to alleviate medical conditions other than pregnancy. Remember, things like genetics, lifestyle factors, access, and individual preference should also be considered when finding the best for you.
At adyn, we work with you to ensure that you find the right for your body with all of those factors in mind.
-
- E.Hormone: A Gateway to Environmental Signaling. Endocrine System: Types of Hormones. Tulane University. (2020). http://e.hormone.tulane.edu/learning/types-of-hormones.html. Accessed 10/2021.
- National Cancer Institute. Reproductive Hormones. NCI Dictionary. https://www.cancer.gov/publications/dictionaries/cancer-terms/def/reproductive-hormone. Accessed 10/2021.
- Planned Parenthood, (n.d.). Birth control methods & OPTIONS: Types of birth control. https://www.plannedparenthood.org/learn/birth-control. Accessed 05/2021-10/2021.
- Jones, Rachel K. “Beyond Birth Control: The Overlooked Benefits of Oral Contraceptive Pills.” Guttmacher Institute, November, 2011 www.guttmacher.org/sites/default/files/report_pdf/beyond-birth-control.pdf
- Office on Women’s Health, US Department of Health and Human Services. Endometriosis. https://www.womenshealth.gov/a-z-topics/endometriosis. Accessed 05/20201-10/2021.
- Brown J, Crawford TJ, Datta S, Prentice A. Oral contraceptives for pain associated with endometriosis. Cochrane Database Syst Rev. 2018 May 22;5(5):CD001019. doi: 10.1002/14651858.CD001019.pub3. PMID: 29786828; PMCID: PMC6494634.
- Schrager S, Larson M, Carlson J, Ledford K, Ehrenthal DB. Beyond Birth Control: Noncontraceptive Benefits of Hormonal Methods and Their Key Role in the General Medical Care of Women. J Womens Health (Larchmt). 2020 Jul;29(7):937-943. doi: 10.1089/jwh.2019.7731. Epub 2020 Mar 5. PMID: 32155101.
- Casper, R. F. (2017). Progestin-only pills may be a better first-line treatment for endometriosis than combined estrogen-progestin contraceptive pills. Fertility and Sterility, 107(3), 533–536. https://doi.org/10.1016/j.fertnstert.2017.01.003
- Grandi G, Barra F, Ferrero S, Sileo FG, Bertucci E, Napolitano A, Facchinetti F. Hormonal contraception in women with endometriosis: a systematic review. Eur J Contracept Reprod Health Care. 2019 Feb;24(1):61-70. doi: 10.1080/13625187.2018.1550576. Epub 2019 Jan 21. PMID: 30664383.
- Soares GM, Vieira CS, de Paula Martins W, Dos Reis RM, de Sá MF, Ferriani RA. Metabolic and cardiovascular impact of oral contraceptives in polycystic ovary syndrome. Int J Clin Pract. 2009 Jan;63(1):160-9. doi: 10.1111/j.1742-1241.2008.01877.x. Epub 2008 Sep 13. PMID: 18795969.
- Calhoun AH, Batur P. Combined hormonal contraceptives and migraine: An update on the evidence. Cleve Clin J Med. 2017 Aug;84(8):631-638. doi: 10.3949/ccjm.84a.16033. PMID: 28806162.
- Sacco S, Merki-Feld GS, Ægidius KL, Bitzer J, Canonico M, Kurth T, Lampl C, Lidegaard Ø, Anne MacGregor E, MaassenVanDenBrink A, Mitsikostas DD, Nappi RE, Ntaios G, Sandset PM, Martelletti P; European Headache Federation (EHF) and the European Society of Contraception and Reproductive Health (ESC). Hormonal contraceptives and risk of ischemic stroke in women with migraine: a consensus statement from the European Headache Federation (EHF) and the European Society of Contraception and Reproductive Health (ESC). J Headache Pain. 2017 Oct 30;18(1):108. doi: 10.1186/s10194-017-0815-1. Erratum in: J Headache Pain. 2018 Sep 10;19(1):81. PMID: 29086160; PMCID: PMC5662520.
- Arowojolu AO, Gallo MF, Lopez LM, Grimes DA. Combined oral contraceptive pills for treatment of acne. Cochrane Database Syst Rev. 2012 Jul 11;(7):CD004425. doi: 10.1002/14651858.CD004425.pub6. PMID: 22786490.
- Jareid M, Thalabard JC, Aarflot M, Bøvelstad HM, Lund E, Braaten T. Levonorgestrel-releasing intrauterine system use is associated with a decreased risk of ovarian and endometrial cancer, without increased risk of breast cancer. Results from the NOWAC Study. Gynecol Oncol. 2018 Apr;149(1):127-132. doi: 10.1016/j.ygyno.2018.02.006. Epub 2018 Mar 2. PMID: 29482839.