Birth control and your period
Hormonal directly impacts your menstrual cycle. Exactly how affects you is different for everyone and depends on which you are taking. can help control periods that are very heavy, long-lasting, unpredictable, or come with other negative symptoms like cramps and nausea. Some people love using it to occasionally skip a period or avoid a monthly period altogether. Unfortunately, sometimes taking can make your period irregular (including ) or have other unwanted side effects.
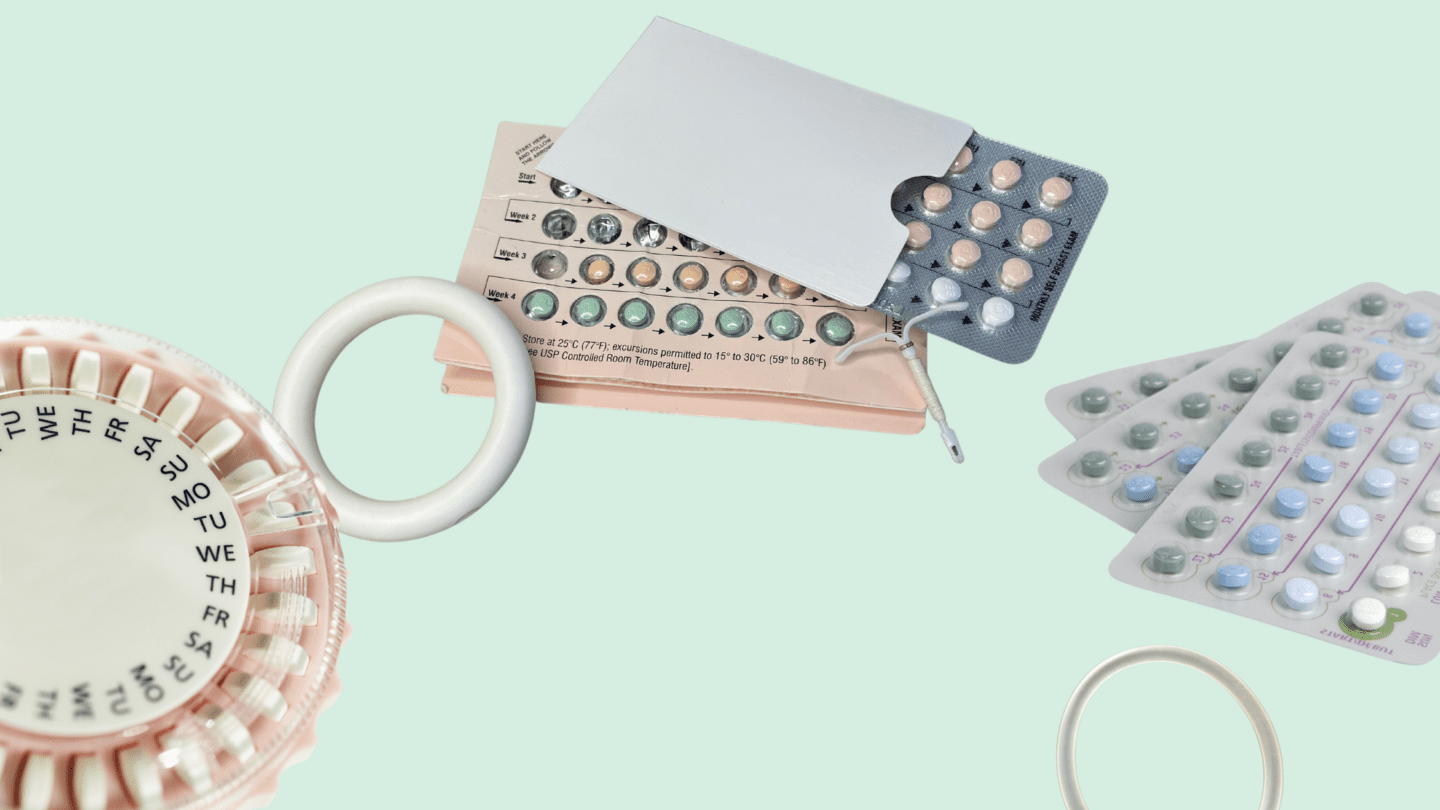
The FDA approved the first birth control pills over 50 years ago. Since then, a wide variety of methods have become available, including:
- The patch
- The ring
- The shot
- The implant
- Intrauterine devices (IUDs)1
In general, these options work similarly, by providing your body with synthetic hormones to prevent pregnancies. Here, we will focus on the combination birth control pill, briefly reviewing how it works before explaining how it impacts your period.
How the (combined) birth control pill works
For this article, we’ll focus on the combination birth control pill.
The combination pill contains a combination (hence its name) of the two reproductive hormones, estrogen and . For the combination pill to be effective, you take one pill at the same time each day, in a series of “active” pills and “inactive” (sometimes referred to as ) pills, or consecutive “active” pills without pause.2
When they occur naturally in your body, and play roles in regulating processes like puberty, pregnancy and childbirth.
Progestins are synthetic (human-made) s that are found in hormonal birth controls. primarily prevents pregnancy by preventing ovulation— it decreases the release of other reproductive hormones that typically cause ovulation. also changes cervical mucus to reduce the ability of sperm to travel and fertilize an egg.3
Synthetic forms of found in combination hormonal birth controls complement the actions of the s by regulating other reproductive hormones to prevent ovulation as well as build up of the uterine lining.3-4
Do I get a “real” period on the contraceptive pill?
In short, no – not technically. The bleeding you get when you’re on the pill is not the same as a menstrual period because there is a different pattern of hormones driving the changes. There is also no egg to shed when you are on the combination pill because ovulation is prevented.5
The bleeding you get when you’re on the pill is not the same as a menstrual period because there is a different pattern of hormones driving the changes.
Instead, the vaginal bleeding that you do have is referred to as a withdrawal bleed. This menstrual-like bleeding occurs while you take the “inactive” pills. Even though it is technically different from a period, you can still have a withdrawal bleed on a regular schedule.
What is my cycle like when on ?
Normally, your body’s reproductive hormones change throughout the month as it prepares for and completes ovulation, prepares the for a possible fertilized egg, then sheds the extra when there is no fertilized egg. During this normal menstrual cycle, a rise in builds up your uterine lining () to prepare for pregnancy. When you don’t get pregnant, that uterine lining sheds as your period.
But, when the hormones in the combination pill prevent your from preparing and releasing eggs, they are also stopping the usual hormonal “cycling”. The hormonal cycling that does happen is because of hormones in the pill and the schedule of “active” and “inactive” pills that you take.
Like what you’re reading? Get the latest straight to your inbox 💌
Birth control pills used to be exclusively packaged with 21 days of active pills and seven days of inactive pills.6 This timing mimics the average length of ~28 days per menstrual cycle. However, now there are a wider variety of options.7 Different options have different effects on your cycle and the frequency and duration of the withdrawal bleed. Besides the 21/7 option, there is also an option for 24 days of active pills and four days of inactive pills. With this option, since there are fewer inactive pills spaced farther apart, it is likely that your withdrawal bleed might be slightly farther apart and shorter.
Extended cycle pill regimens contain active pills for about three months, with inactive/low-dose pills for one week, during which you have a withdrawal bleed. So with this type of combination pill, you have a “period” only four times a year.
Skipping your withdrawal bleed
You can also use the combination pill to skip your withdrawal bleed all together. Skipping your withdrawal bleed is safe for most people who are already on . Some people skip their bleed for convenience, but you could also skip it if the monthly hormonal cycling leaves you suffering from symptoms like cramps, fatigue and migraines.8 The simplest way is probably to use the combination pills that come in continuous active pill versions– without any inactive pills, your monthly bleed eventually goes away or becomes very light.2
You can also safely skip your withdrawal bleed if you are (already) taking the monthly type of combination pill. To do that, you just skip taking the inactive pills and instead move directly on to a new month of active pills. You can use this to skip a period strategically — like for a big event or trip. If you already use a combination pill that works for you, you wouldn’t need to change s to skip your monthly bleeding.
One disadvantage of skipping your withdrawal bleed is that you won’t have it as a sign that you are not pregnant. So, if you are having nausea, atypical fatigue or breast tenderness and haven’t had a period or withdrawal bleed, it would make sense to take a home pregnancy test.
Is adyn right for you? Take the quiz.
Breakthrough bleeding and
As the amount of hormones in combination birth control pills has decreased over time, has become more common. is more common with low-dose/ultra-low-dose s and the extended cycle pill regimens.5,9 Breakthrough, or unexpected, bleeding or can be pretty obnoxious, but is generally not a sign of a health problem.10
Most of the time, is light. It occasionally requires sanitary protection, but more often is just . Generally, is not a sign that something is medically wrong. But if you’re worried, it is always best to consult your healthcare provider.
The easiest way to stop is to just keep taking your pills — it usually improves within the first 3-6 months. With the extended cycle or continuous cycle pills, a majority of users stopped having periods by one year of use.7
Also, quitting smoking and being sure to take your birth control pills at the same time each day can also help reduce .9 If you have already done those things, and you have been taking the pill for at least three months, your health care provider might suggest an NSAID (non-steriod anti-inflammatory drug) to help with .9
If you are still having problems with after that point, you may want to try a different type of . We specialize in helping people find the right for their bodies.
If you want a more regular, predictable, or less painful period, our team may be able to help.
-
- Birth Control Methods & Options. Planned Parenthood. https://www.plannedparenthood.org/learn/birth-control. Accessed 10/2021.
- Combination birth control pills. The Mayo Clinic. https://www.mayoclinic.org/tests-procedures/combination-birth-control-pills/about/pac-20385282. Accessed 10/2021.
- Cooper DB, Mahdy H. Oral Contraceptive Pills. https://www.ncbi.nlm.nih.gov/books/NBK430882/https://www.ncbi.nlm.nih.gov/books/NBK430882/. [Updated 2021 Aug 25]. Accessed 10/2021.
- Birth control pill FAQ: Benefits, risks and choices. The Mayo Clinic. https://www.mayoclinic.org/healthy-lifestyle/birth-control/in-depth/birth-control-pill/art-20045136. Accessed 10/2021.
- Wright, K. P., & Johnson, J. V. (2008). Evaluation of extended and continuous use oral contraceptives. Therapeutics and clinical risk management, 4(5), 905–911. https://doi.org/10.2147/tcrm.s2143
- Schrager, S. (2002). Abnormal Uterine Bleeding Associated with Hormonal Contraception. Am Fam Physician. 2002 May 15;65(10):2073-2081.